phlebitis
Recognising phlebitis
& treat
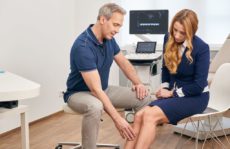
Superficial phlebitis (thrombophlebitis) should be recognised as never trivialised become. If the skin over a superficial vein reddens, there is a distinct feeling of warmth locally, the affected vein swells and hardens, it is high time to see a specialist. If left untreated, an initially superficial thrombosis can develop into a thrombosis of the deep veins and even - albeit rarely - into a potentially life-threatening pulmonary embolism.
The therapy
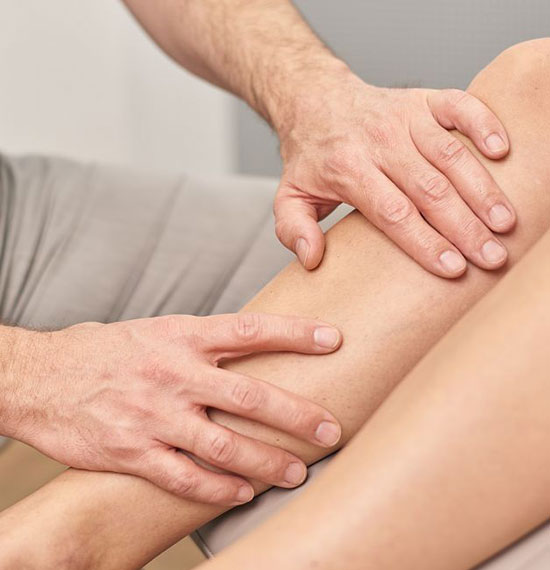
Treatment with compression and blood thinning
The causes of superficial phlebitis can be varied, depending on whether the affected vein was previously healthy or the inflammation occurs together with a varicose vein or other symptoms.
I more severe the inflammation the longer the duration of treatment. In most cases Local cooling measures and a Compression therapy in combination with anti-inflammatory and blood-thinning medication.
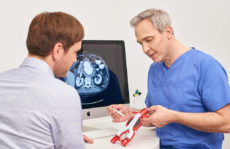
The cause of the inflammation and clot formation must also be clarified.
Frequently asked questions on the topic of "phlebitis"
Superficial phlebitis can be recognised by the classic signs such as redness, swelling, overheating and hardening of the vein with localised tenderness. Further ultrasound examination then clarifies whether there is a blood clot (thrombus) in the affected vein, which closes the vein from the inside and thus irritates the vein (most common variant) or whether there is inflammation of the vein wall without a blood clot (rare variant). This is important in order to initiate the appropriate therapy, as the presence of a clot often requires blood thinning with medication over a certain period of time, which is not necessary in the variant without a clot.
In the case of pure phlebitis, pain-relieving medication is given and a cooling bandage is applied. If there is also a clot in the vein (thrombus), if the clot is more than 5 cm long, a blood thinner is administered for 6 weeks in the form of injections or tablets. To alleviate the symptoms, a compression bandage or compression stocking can be applied and the affected vein cooled.
If you have phlebitis, you should always consult a doctor, as only an ultrasound scan can determine the true extent of the inflammation and any blood clot (thrombus) that may be present in the vein at the same time. Without adequate treatment, superficial phlebitis can also lead to deep vein thrombosis (or has already done so).
As the name suggests, deep vein thrombosis affects the veins in the deeper layers of the limb that are not visible from the outside and - in contrast to superficial vein thrombosis - leads to a thrombosis of the veins.
Deep vein thrombosis - usually always leads to swelling of the affected limb (leg or arm). Deep vein thrombosis harbours an increased risk of pulmonary embolism if the clot detaches from the vein and is washed away into the pulmonary circulation. Superficial vein thrombosis can also lead to a pulmonary embolism, although in many rarer cases. The difference between superficial and deep vein thrombosis therefore lies in the threat to the patient and in further treatment. Small superficial vein thromboses are usually only treated with painkillers or, if they are more than 5 cm long, with blood thinners for 6 weeks, whereas deep vein thrombosis usually requires at least 3 months of anticoagulation (blood thinning) in tablet or injection form.
Superficial phlebitis with a clot in the vein usually heals without any problems within a few weeks. If there is no clot in the vein and the vein wall is only irritated, the healing process is usually faster.